An Atlas of Lumps and Bumps, Part 48: Olecranon Bursitis
Olecranon Bursitis
The olecranon bursa is a superficial bursa located immediately posterior to the olecranon process of the ulna bone and triceps tendon and loosely connected to the overlying skin in the elbow area.1,2 The bursa serves as a cushion and allows the olecranon process to glide smoothly across the overlying tissues with extension and flexion of the elbow.1 Olecranon bursitis refers to inflammation of the bursa, which can be non-septic or septic.3
By far, the most common cause of non-septic olecranon bursitis is trauma, which can lead to intrabursal bleeding and release of inflammatory mediators, resulting in an overproduction of bursal fluid.2,3 Truama may result from direct injury, overuse either in athletes (e.g., wrestlers, gymnasts, volleyball players), individuals in certain manual labor occupations (e.g., carpenters, carpet layers, roofers, gardeners, auto mechanics, plumbers), or repetitive minor trauma (e.g., prolonged pressure on the elbow or constantly rubbing of the elbow against a table [student’s elbow]).3-5 Other causes that are associated with non-septic olecranon bursitis include rheumatoid arthritis, psoriatic arthritis, systemic lupus erythematosus, gout, diabetes mellitus, uremia, calcium pyrophosphate deposition disease (also known as articular chondrocalcinosis), drug abuse, alcohol abuse, immonosuppression, and human immunodeficiency virus (HIV) infection.2,6-9
Septic olecranon bursitis accounts for approximately 20% of cases of olecranon bursitis.7 The infection is usually via a transcutaneous route such as direct inoculation of the microorganism into the bursa through a wound or local spread from nearby cellulitis.2 Hematogenous spread is extremely rare because the bursa has a poor blood supply.2 Septic olecranon bursitis is most commonly caused by Staphylococcus aureus (responsible for approximatley 80% of cases) , followed by Staphylococcus epidermidis and Streptococcus pyogenes.2,6,7 Polymicrobial infections have been reported in approximately 10% of cases of bacterial olecranon bursitis.2 Olecranon bursitis caused by fungi is rare.10,11 Up to 50% of cases of septic olecranon bursitis occur in immunocompromised individuals.3
The exact incidence of olecranon bursitis is not known. It is estimated that olecranon bursitis accounts for 1 to 10 cases per 10,000 hospital admissions and approximately 3 per 1000 visits to emegency departments.2,8 Approximately 80% of cases are non-septic.4,7 Olecranon bursitis occurs in individuals of all age group with a peak incidence between 30 to 60 years of age.7 The male to female ratio is approximately 4:1.3
Clinically, olecranon bursitis presents as a fluctuant, well-demarcated swelling/lump simulating a goose egg or golf ball over the olecranon process in the posterior elbow area (Figure 1).1,2
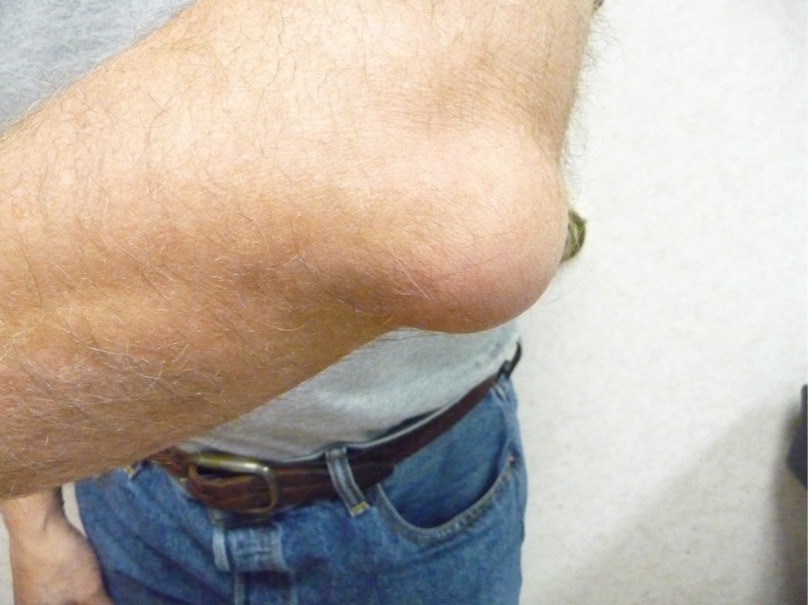
Fig. 1. Olecranon bursitis presents as a fluctuant, well-demarcated swelling/lump simulating a goose egg or golf ball.
Full elbow range of motion is generally preserved in septic and non-septic olecranon bursitis (Figure 2), but pain is noted in extension and flexion with septic olecranon bursitis.2
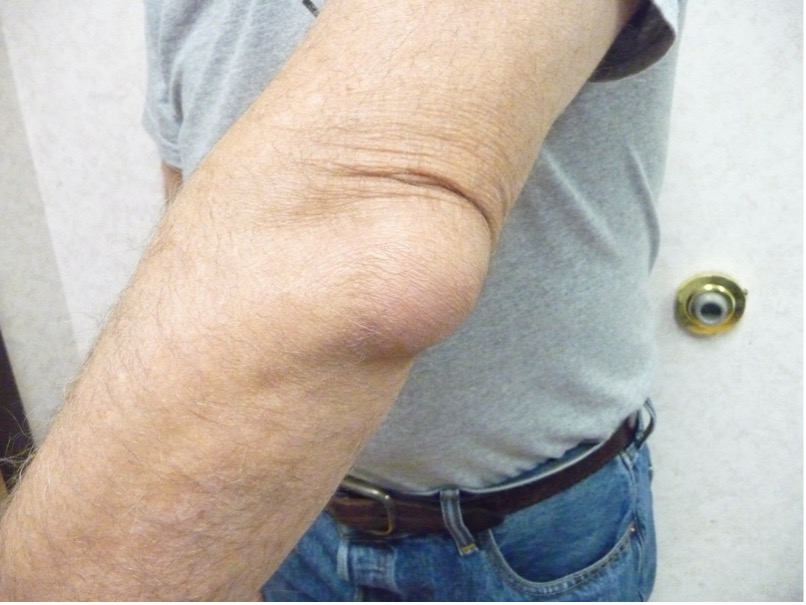
Fig. 2. Full elbow range of motion is generally preserved in septic and non-septic olecranon bursitis.
History of immunodeciency/immunosuppression and physical findings of fever (temperature > 37.8oC), olecranon bursal warmth (temperature difference ≥ 2.2 oC between the affected bursa and contralateral bursa), tenderness over the swelling/lump (Figure 3), and nearby skin lesions (e.g., cellulitis, wound) suggest septic olecranon bursitis.3
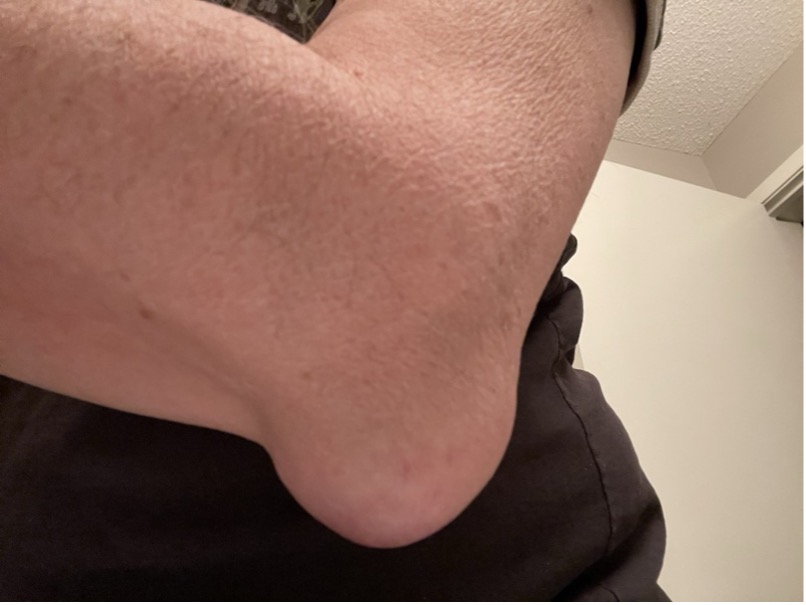
Fig. 3. History of immunodeciency/immunosuppression and physical findings of fever, olecranon bursal warmth, tenderness over the swelling/lump, and nearby skin lesions suggest septic olecranon bursitis.
Underlying medical conditions such as rheumatoid arthritis and gout favor non-septic olecranon bursitis. Erythema of the overlying skin occurs in 63% to 100% of cases of septic bursitis and 25% of patients with non-septic olecranon bursitis, respectively.8
The diagnosis is usually based on clinical findings. Confirmation with aspiration and gram-stain and culture of the bursal fluid may be considered as the gold standard for diagnosing septic olecranon bursitis is a positive culture of the bursal fluid.1,2,6 Imaging studies are usually not necessary but radiographs of the elbow should be considered if olecranon fracture is suspected.2,8
Complications of olecranon bursitis include secondary bacterial infection and entrapment neuropathy (e.g., ulnar neuropathy).12
AUTHORS:
Alexander K.C. Leung, MD1,2, Benjamin Barankin, MD3, Joseph M. Lam, MD4, Alex H.C. Wong, MD5, Kin Fon Leong, MD6
AFFILIATIONS:
1Clinical Professor of Pediatrics, the University of Calgary, Calgary, Alberta, Canada
2Pediatric Consultant, the Alberta Children’s Hospital, Calgary, Alberta, Canada
3Dermatologist, Medical Director and Founder, the Toronto Dermatology Centre, Toronto, Ontario, Canada
4Associate Clinical Professor of Pediatrics, Dermatology and Skin Sciences, the University of British Columbia, Vancouver, British Columbia, Canada.
5Department of Family Medicine, The University of Calgary, Calgary, Alberta, Canada
6Pediatric Dermatologist, the Pediatric Institute, Kuala Lumpur General Hospital, Kuala Lumpur, Malaysia
CITATION:
Leung AKC, Barankin B, Lam JM, Wong AHC, Leong KF. An Atlas of Lumps and Bumps, Part 48: Olecranon Bursitis. Consultant. 2025;65(2):eXX. doi: 10.25270/con.2025.02.000002.
CORRESPONDENCE:
Alexander K. C. Leung, MD, #200, 233 16th Ave NW, Calgary, AB T2M 0H5, Canada (aleung@ucalgary.ca)
EDITOR’S NOTE:
This article is part of a series describing and differentiating dermatologic lumps and bumps. To access previously published articles in the series, visit: https://www.consultant360.com/resource-center/atlas-lumps-and-bumps.
References
- Pangia J, Rizvi TJ. Olecranon bursitis. In: StatPearls [Internet]. Treasure Island, FL: StatPearls Publishing; 2021 Jan–. PMID: 29262058. Available from: https://www.ncbi.nlm.nih.gov/books/NBK441895/ (Include direct URL if available).
- Reilly D, Kamineni S. Olecranon bursitis. J Shoulder Elbow Surg. 2016;25(1):158-167. doi:10.1016/j.jse.2015.08.032.
- Baumbach SF, Lobo CM, Badyine I, Mutschler W, Kanz KG. Prepatellar and olecranon bursitis: literature review and development of a treatment algorithm. Arch Orthop Trauma Surg. 2014;134(3):359-370. doi:10.1007/s00402-013-1882-7.
- Harris-Spinks C, Nabhan D, Khodaee M. Noniatrogenic septic olecranon bursitis: report of two cases and review of the literature. Curr Sports Med Rep. 2016;15(1):33-37. doi:10.1249/JSR.0000000000000220.
- Schermann H, Karakis I, Dolkart O, Maman E, Kadar A, Chechik O. Olecranon bursitis in a military population: epidemiology and evidence for prolonged morbidity in combat recruits. Mil Med. 2017;182(9):e1976-e1980. doi:10.7205/MILMED-D-16-00402.
- Blackwell JR, Hay BA, Bolt AM, Hay SM. Olecranon bursitis: a systematic overview. Shoulder Elbow. 2014;6(3):182-190. doi:10.1177/1758573214532787.
- Deal JB Jr, Vaslow AS, Bickley RJ, Verwiebe EG, Ryan PM. Empirical treatment of uncomplicated septic olecranon bursitis without aspiration. J Hand Surg Am. 2020;45(1):20-25. doi:10.1016/j.jhsa.2019.06.012.
- Del Buono A, Franceschi F, Palumbo A, Denaro V, Maffulli N. Diagnosis and management of olecranon bursitis. Surgeon. 2012;10(5):297-300. doi:10.1016/j.surge.2012.02.002.
- Patel J, Girishkumar, Mruthyunjaya, Rupakumar CS. Bilateral olecranon bursitis—a rare clinical presentation of calcium pyrophosphate crystal deposition disease. J Orthop Case Rep. 2014;4(1):3-6. doi:10.13107/jocr.2250-0685.137.
- Gamarra-Hilburn CF, Rios G, Vilá LM. Olecranon bursitis caused by Candida parapsilosis in a patient with rheumatoid arthritis. Case Rep Rheumatol. 2016;2016:2019250. doi:10.1155/2016/2019250.
- Guevara-Suarez M, Llaurado M, Pujol I, Mayayo E, Martin-Vicente A, Gené J. Fungal olecranon bursitis in an immunocompetent patient by Knoxdaviesia dimorphospora sp. nov.: case report and review. Mycopathologia. 2018;183(2):407-415. doi:10.1007/s11046-017-0211-z.
- Yamazaki H, Shinone M, Kato H. Compressive ulnar neuropathy caused by olecranon bursitis and concomitant epidermal cyst: a case report. J Hand Surg Asian Pac Vol. 2017;22(4):503-507. doi:10.1142/S0218810417720339.


