Peer Reviewed
Atypical Presentation of a Subacute Temporal Infarct
Introduction. A 69-year-old man presented to the emergency department (ED) with a dull, but worsening headache.
History. The patient's medical history includes non-ST-segment elevation myocardial infarction (NSTEMI), type 2 diabetes mellitus, prostate cancer, and transient ischemic attack. The patient stated that the headache started 4 days prior to presentation and was constant in duration, increasing in intensity upon waking each day. The patient stated that the headache was accompanied by brief bouts of dysphasia, in which he would forget how to say, “a word or two.”
The patient denied any other signs or symptoms at the time of the event, including facial drooping, diplopia, aphasia, vertigo, paralysis, fever, chills, head injury, and history of migraines. The patients’ medications at the time included clopidogrel 75 mg daily, aspirin 81 mg daily, sitagliptin 25 mg daily, metformin 1000 mg twice a day, atorvastatin 20 mg daily, and metoprolol 25 mg daily. The headache remained a consistent pain level but changed location from the bilateral temples to behind his right eye. It was the worst headache he ever experienced, the patient said.
The patient’s blood pressure (BP) was 129 systolic and 90 diastolic. His temperature was 98.7˚F. He had a respiratory rate of 16/minute and a 98% resting oxygen saturation level. His physical examination showed that his cardiac, pulmonary, head, eyes, ears, nose, and throat (HEENT), and neurological tests were all within normal ranges. The patient’s National Institutes of Health Stroke Scale (NIHSS) score was 0, and his blood glucose was in the 270s.
The ED course of action consisted of administration of intravenous (IV) fluids, medication for headache, and computed tomography (CT) scan. The decision to admit the patient to the hospital was reached by the emergency department team after his brain CT visualized an acute infarct. Although no acute events occurred in the hospital, the hospitalist ordered transesophageal echocardiogram (TEE) and consulted neurology.
During this time, the patient admitted to the hospitalist that he forgot to take his clopidogrel and aspirin “for some time”. Neurology found no focal deficits and recommended continuation of clopidogrel, aspirin, and statin as well as head and neck computed tomography angiography (CTA) following the patient’s MRI results. After the scans, the patient was discharged the next day with follow-ups to radiology/oncology and family medicine both in 1 month.
Diagnostic testing. The CT brain scan in the ED showed local mass effect and hypoattenuation in the right temporal lobe (Fig. 1). The MRI confirmed an acute to subacute infarct, which was cortically restricted and spanned to the superior temporal lobe and insula (Fig. 2). The echocardiogram reflected mild concentric left ventricle hypertrophy with ejection fraction of 51, left anterior descending artery regional wall motion abnormalities, and normal right ventricle function. The outpatient head and neck CTA showed a stable non-hemorrhagic infarct without herniation.
Differential Diagnosis. Imaging found temporal infarct as the most likely diagnosis for this patient’s headache. Other differential diagnoses include thromboembolic stroke, subdural hematoma, arteriovenous malformations, intracranial tumor, carbon monoxide poisoning, abscess, meningitis, hypertensive emergency, complex migraine, and cluster headache. The patient did not exhibit systematic signs or meet systemic inflammatory response syndrome criteria, so it was an unlikely infectious etiology. The patient’s vital signs were within normal limits, so a hypertensive emergency was unlikely. Migraine would be a diagnosis of exclusion. The rest of the differentials need visualization to ruled out.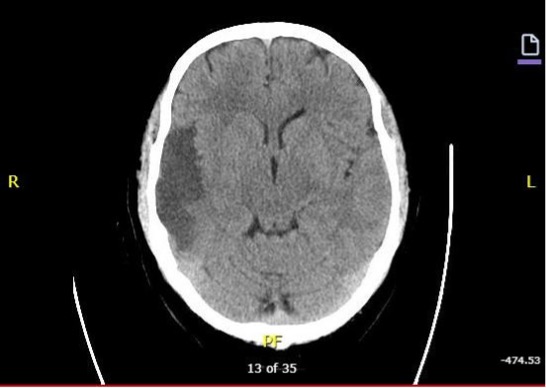
Figure 1. CT asserts local mass effect and hypoattenuation with loss of gray/white matter at the right temporal lobe.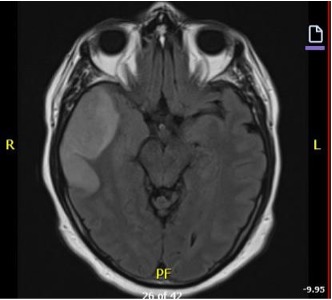
Figure 2. MRI illuminated cortical and subcortical lesion within the right temporal lobe that extends to the right insula.
Treatment and management. The patient was admitted to the hospital floor, given IV fluids, and received lorazepam 0.25 mg once, ondansetron 4 mg injection once, and IV magnesium sulfate 1 g at 100mL/hr once for headache management. He also received levofloxacin 500 mg twice, which was administered in the hospital to cover for infectious etiology of stroke. The patient’s TEE revealed no need for long-term anticoagulation.
Neurology administered serial neurologic examinations and advised neuroprotective orders such as avoiding hypotonic solutions, normalizing magnesium levels, and avoiding clonidine. Neurologic examination revealed no change from baseline. Consultants for physical, occupational, and speech therapy all recommended home discharge when medically cleared. The patient’s stroke was deemed stable medically since there were no symptoms nor actionable items found on hos scans. He was discharged on his home regimen and ambulatory telemetry to follow-up with family medicine and urology in 1 month.
Outcome and follow-up. On follow-up to primary care, the patient did not present with typical stroke symptoms. His physical examination revealed residual word finding and fatigue. His headache etiology was most likely from stroke versus migraine, meningitis, venous thrombosis, or temporal arteritis. Based on past medical history of NSTEMI, stroke, and internal carotid artery (ICA) stenosis, it was recommended by primary care provider to obtain an ICA duplex to evaluate for further progression of stenosis. His ICA duplex showed 20% to 39% bilateral internal carotid stenosis. This indicates mild bilateral stenosis since both are less than <50 %.
Discussion. The current literature describes common characteristics among headaches secondary to acute stroke. Headache can present as the only symptom of stroke in certain cases without other neurologic defects.⁴ Women experience this symptom of stroke more often than men.² Pertinent history for evaluating stroke includes a new type of headache in an individual, especially a new type of migraine.⁵,⁶ Eighty-six percent of patients experience headache on Day 1 of the stroke, but it can persist as long as 8 days.⁷ The pain is generally described as pulsating or throbbing in the back of the head.⁷ These characterized strokes are more frequent in strokes with lower NIHSS scores,³ and they most frequently present with posterior circulation and embolic strokes.4-6 The prevailing theories are related to an abundance of nociceptive nerve endings in the vasculature corresponding to the patients' reported pain, cytokine expression, and reduced blood flow.1,4,6 Embolisms larger than 15 mm produced symptoms theoretically secondary to vasodilation by local cytokines. Still the exact mechanisms remains a gap in our knowledge.
Conclusion. This patient endured a new onset headache of 4 days duration, which reflected acute to subacute temporal infarct. His past medical history of NSTEMI, prostate cancer, and TIA underscores a history of hypercoagulability, exacerbated by forgetting to take his plavix and aspirin. His headache was neither throbbing nor pulsating but consistently increased in intensity. The headache also corresponded with a lower NIHSS score. Imaging reflected an infarct that was older than 24 hours, possibly starting at the time of headache onset. Uniquely, the infarct was not present in posterior circulation and no evidence of cardioembolic score was identified on echocardiogram. The challenge of this case presenting in family medicine and emergency medicine offices is deciding whether to get a CT scan. Low NIHSS score might point a physician away from stroke, but the literature supports the use of CT head in his patient, and further investigation is needed to evaluate nonspecific headaches in those in high risk of thromboembolic events. The patient’s medical history included consistent posterior pain, throbbing or pulsating pain, and headache, all of which should point toward CT scan, especially in someone with several risk factors. This case demonstrates the importance of getting a thorough headache history, referring to the red flags for headaches, and assessing drug compliance in at-risk individuals with headache.
AUTHORS:
Rei Kola, OMS IV1 • Joseph Mandato, OMS IV1 • Robert Bales, MD, MPH, FAAFP2
AFFILIATIONS:
1Ohio University Heritage College of Osteopathic Medicine, Cleveland, OH
2Department of Family Medicine, Cleveland Clinic, Cleveland, OH
CITATION:
Kola R, Mandato J, Bales R. Atypical Presentation of a Subacute Temporal Infarct. Consultant. Published online: February 14, 2025. DOI: 10.25270/con.2025.03.000005
Received September 4, 2024. Accepted October 28, 2024.
DISCLOSURES:
The authors report no relevant financial relationships.
ACKNOWLEDGEMENTS:
None.
CORRESPONDENCE:
Robert Bales, MD, Cleveland Clinic South Pointe Department of Family Medicine, 2000 Harvard Avenue, Warrensville, OH 44122 (Balesr@ccf.org)
References
Ge Y, Dong W, Lu H, Zhang X, Huang S, Yang Y, Ni J. Association of concomitant headache with hypoperfusion in ischemic stroke: A multimodal CT-based study. Clin Transl Sci. 2022;15(12):2868-2877. doi:10.1111/cts.13405.
Harriott AM, Karakaya F, Ayata C. Headache after ischemic stroke: A systematic review and meta-analysis. Neurology. 2020;94(1):e75-e86. doi:10.1212/WNL.0000000000008591.
Hussein M, Ali M, Abdelghaffar M, et al. Frequency, characteristics, and predictors of headache attributed to acute ischemic stroke. Rev Neurol (Paris). 2023;179(9):1000-1007. doi:10.1016/j.neurol.2023.03.022.
Jamieson DG, Cheng NT, Skliut M. Headache and acute stroke. Curr Pain Headache Rep. 2014;18(9):444. doi:10.1007/s11916-014-0444-1.
Lebedeva ER, Ushenin AV, Gurary NM, et al. Headache at onset of first-ever ischemic stroke: Clinical characteristics and predictors. Eur J Neurol. 2021;28(3):852-860. doi:10.1111/ene.14684.
Lebedeva ER, Ushenin AV, Gurary NM, Gilev DV, Olesen J. Sentinel headache as a warning symptom of ischemic stroke. J Headache Pain. 2020;21(1):70. doi:10.1186/s10194-020-01140-3.
Verdelho A, Ferro JM, Melo T, Canhão P, Falcão F. Headache in acute stroke: A prospective study in the first 8 days. Cephalalgia. 2008;28(4):346-354. doi:10.1111/j.1468-2982.2007.01514.x.


