How is urinary tract infection best managed in elderly persons?
THE CASE
An 83-year-old woman is brought by her daughter for evaluation because of increasing confusion during the past few days. The patient has early Alzheimer dementia, hypertension, and type 2 diabetes. She takes donepezil, 10 mg/d; lisinopril, 5 mg/d; and glipizide, 5 mg bid. She is unable to bathe and dress herself as well as previously, has been crying for no apparent reason, and has lost her appetite.
The patient has lost 6 lb in the past 3 weeks and appears more anxious and confused than usual. Her score on the Mini-Mental State Examination is 18, a loss of 3 points since the last visit. She is afebrile; her heart rate is 92 beats per minute. Palpation of the abdomen elicits slight wincing. There is no costovertebral angle tenderness. Lungs are clear and skin is intact. The remainder of the examination is unremarkable.
A complete blood cell (CBC) count, chemistry 7 panel, and urinalysis with culture and sensitivity determination are ordered. A chest radiograph is not ordered because there are no localizing symptoms. No treatment is given on the day of evaluation. The patient’s daughter is told to watch for heightened confusion and to be sure her mother’s fluid intake is increased pending results of laboratory testing.
Acute confusion in elderly persons, especially those with dementia, has a wide differential diagnosis. The most common causes are infection (principally respiratory tract, urinary tract, or skin); new medications; and electrolyte disturbance. Because this patient had not started any new medications, the laboratory workup is likely to be revealing.
Laboratory results show a normal CBC count with no leukocytosis. The chemistry 7 panel reveals a slightly higher blood urea nitrogen level than usual (24 vs 15 mg/dL) and a normal serum creatinine level, which indicates mild dehydration. The urinalysis shows bacteriuria and pyuria; culture results are pending.
How is urinary tract infection (UTI) best managed in elderly persons?
Genitourinary infection is the second most common type of infection in community-dwelling adults older than 65 years; it occurs only slightly less frequently than upper respiratory tract infection. 1 The presentation of UTI in elderly patients may differ significantly from that in younger ones. Chronic urinary symptoms are common in elderly persons, and the classic triad of UTI-frequency, urgency, and dysuria-occurs routinely in older persons without infection.2 As many as one third of community- dwelling elderly women are incontinent, which can further confuse the presentation. A high index of suspicion is needed first to entertain the diagnosis and then to pursue a thorough evaluation.
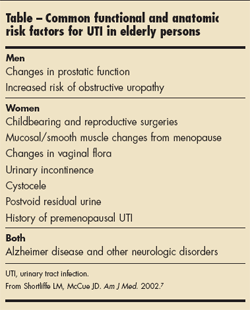
A variety of risk factors predispose older persons to UTIs (Table). In those between ages 50 and 70 years, the most common are urinary tract surgery, incontinence, cystocele, high postvoid residual volume, and low estrogen levels. Neurogenic conditions of the bladder—particularly those associated with diabetes and with anticholinergic medication—alsopredispose to UTI.3 In patients older than 70 years, risk factors include the use of multiple antibiotics, the presence of an indwelling catheter, and a history of UTI.
The range of potential uropathogens in elderly patients is considerably broader than in the younger adult population; this diversity requires that cultures be obtained in all elderly persons with UTI. Escherichia coli is the predominant culprit organism in persons younger than 50 years, but it is responsible for fewer than half of UTIs in older persons. Other potential culprits include gram-negative organisms such as Proteus, Serratia, Klebsiella, and Pseudomonas. Grampositive organisms, such as Enterococcus and coagulase-negative staphylococci, are frequent isolates, as is Candida. 4 Many UTIs in elderly persons are polymicrobial.
DIAGNOSIS
UTI in elderly persons presents in various ways. In a relatively young, healthy older person, the classic triad is usually present. In patients who are older than 75 years and less robust, however, the predominant symptoms are found outside of the urinary tract. A decline in functional ability, weight loss, and delirium are common presentations. In a patient with dementia, worsening confusion and behavioral problems may be the only indication of a possible UTI. The patient may be afebrile. There may be a diminished level of alertness; however, this should not be assumed to indicate sepsis. Flank tenderness may or may not be present; vague abdominal tenderness is common.
The diagnosis of UTI requires an appropriate constellation of symptoms, which may be localized to the urinary tract or outside it; identification of a recognized pathogen on culture; bacteriuria (more than 105 colony forming units [CFU]/mL); and evidence of white blood cells in the urine. It can be difficult to obtain a clean urine specimen in an elderly patient. Nearly 30% of clean-catch specimens are contaminated.5 A specimen obtained by catheterization is more reliable, and this method is therefore recommended.
MANAGEMENT
Treat all UTIs in persons older than 65 years as if they are complicated. (Complicated UTIs occur in persons with urinary abnormalities, are more frequently associated with non–E coli gram-negative organisms, and are more likely to be resistant to standard therapy and to be associated with serious sequelae such as pyelonephritis or sepsis.) UTIs in older adults—as well as in younger men—require a longer duration of antibiotic therapy than UTIs in young women, who usually have uncomplicated infections.
Empiric therapy in elderly women is generally initiated with trimethoprim- sulfamethoxazole (TMP-SMX) or a fluoroquinolone. One study found a cure rate of 96% with ciprofloxacin compared with 87% with TMP-SMX.5 The latter agent was also associated with more side effects and had a higher discontinuation rate than ciprofloxacin. Ciprofloxacin and levofloxacin are the most commonly prescribed fluoroquinolones for UTI. Although both are effective, ciprofloxacin has a higher potential for drug interactions and has occasionally been associated with delirium.5 Levofloxacin may therefore be the preferred empiric choice. Treatment is generally continued for at least 10 days.
Fluoroquinolones have superior prostate penetration and are therefore the recommended agents for empiric therapy in elderly men. Therapy can be tailored when culture results are known. Treatment is generally continued for a minimum of 14 days.
Appropriate treatment generally results in cure. However, relapse and recurrence are common, and repeated cultures should be performed, if possible, to ascertain that the organism has been eradicated.
UTI IN INSTITUTIONALIZED ELDERLY PERSONS
These patients, whether in longterm– care facilities or hospitals, are more likely to have indwelling catheters and urologic abnormalities that predispose to more frequent and potentially more serious infections. Significant comorbidities, such as dementia, malnutrition, immunosuppression, pressure ulcers, and the presence of a feeding tube, may complicate diagnosis and treatment. Because these patients are less likely to be able to describe specific urinary problems, the staff must be on the alert for other symptoms of UTI in order to avoid serious sequelae such as pyelonephritis, prostatitis, and sepsis. Finally, inadequate hand-washing techniques, primarily among staff, can spread microorganisms throughout the institution.
The incidence of antimicrobial resistance is higher in institutionalized patients (Box); therefore, appropriate cultures must be obtained and treatment continued for at least 10 to 14 days. Indwelling catheters must be changed at the initiation of therapy; colonization usually occurs within 72 hours.

ASYMPTOMATIC BACTERIURIA
Asymptomatic bacteriuria (ASB) is diagnosed by the positive culture of the same pathogen in 2 clear voided urine specimens from a patient without symptoms. The prevalence of ASB in elderly persons ranges from 17% to 50% in women and 6% to 34% in men; the percentage increases with age, functional status, and the use of indwelling Foley catheters.6 ASB does not appear to contribute to morbidity or mortality. Efforts to sterilize the urine with prolonged antibiotic therapy are futile, because recurrence is the norm. ASB is a benign condition that does not require treatment.
FOLLOW-UP
Recurrent UTI is common in elderly persons, and follow-up cultures are mandatory. A recurrence or relapse is evaluated and treated in the same way as a primary infection, although the duration of antibiotic therapy may be increased. Routine prophylaxis is not recommended, because it may select for more resistant organisms. Complications such as sepsis or pyelonephritis generally require hospitalization and treatment with parenteral antibiotics. Referral to a urologist is indicated when an altered urogenital tract complicates treatment or when eradication of the organism cannot be documented.
OUTCOME OF THIS CASE
The final urine culture revealed more than 105 CFU of E coli sensitive to fluoroquinolones. A 10-day course of levofloxacin, 250 mg/d, was prescribed. Within 48 hours, the patient had regained her appetite, and her ability to perform activities of daily living had returned to normal. Her acute confusion and tearfulness resolved during the course of treatment.
1. Foxman B. Epidemiology of urinary tract infections: incidence, morbidity and economic costs. AmJ Med. 2002;113:5S-13S.
2. Wood CA, Abrutyn E. Urinary tract infection in older adults. Clin Geriatr Med. 1998;14:267-283.
3. Wallach FR. Update on treatment of pneumonia, influenza, and urinary tract infections. Geriatrics. 2001;56:43-47.
4. Nicolle LE. Resistant pathogens in urinary tract infections. J Am Geriatr Soc. 2002;50:S230-S235.
5. Gomolin IH, Siami PF, Reuning-Scherer J, et al. Efficacy and safety of ciprofloxacin oral suspension versus trimethoprim-sulfamethoxazole oral suspension for treatment of older women with acute urinary tract infection. J Am Geriatr Soc. 2001;49:1606-1613.
6. Raz R. Asymptomatic bacteriuria. Clinical significance and management. Int J Antimicrob Agents. 2003;22:S45-S47.
7. Shortliffe LM, McCue JD. Urinary tract infection at the age extremes: pediatrics and geriatrics. Am J Med. 2002;113(suppl 1A):55S-66S.


